Low Blood Pressure Treatments
Find Low Blood Pressure Treatments
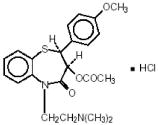
Diltiazem
What is Matzim (Diltiazem)?
Approved To Treat
Top Global Experts
Related Clinical Trials
Summary: This is a small, pilot study with a primary goal of assessing patient perceptions of two medication treatments for supraventricular tachycardia in adult patients treated in the Emergency Department.
Summary: Supraventricular tachycardia (SVT) is a dysrhythmia characterized rapid heart rate, typically with rapid onset. SVT accounts for over 50,000 emergency department visits per year. Of patients with regular, narrow-complex SVT, the mainstay of therapy includes adenosine and diltiazem. Adenosine is recommend by American and European guidelines as first-line therapy, however adenosine carries unique si...
Summary: This study aimed to compare the clinical outcomes of left bundle branch area pacing combined with atrioventricular node ablation and pharmacologic treatment optimized according to guidelines in patients with symptomatic atrial fibrillation refractory or intolerant to drug therapy or catheter ablation.
Related Latest Advances
Brand Information
Patients with sick sinus syndrome except in the presence of a functioning ventricular pacemaker. Patients with second- or third-degree AV block except in the presence of a functioning ventricular pacemaker. Patients with hypotension (less than 90 mm Hg systolic). Patients who have demonstrated hypersensitivity to the drug. Patients with acute myocardial infarction and pulmonary.
- Bradycardia and AV block
- Heart failure
- Acute hepatic injury
- Severe skin reactions
- That the Matzim LA (diltiazem hydrochloride) extended-release tablet should be swallowed whole and not chewed or crushed.
- To consult the physician who prescribed Matzim LA (diltiazem hydrochloride) extended-release tablets before taking or stopping any other medications, including over-the-counter products or nutritional supplements, such as St. John’s wort.
- To contact the physician who prescribed Matzim LA (diltiazem hydrochloride) extended-release tablets or any other physician immediately if they experience possible adverse reactions, including bradycardia, arrhythmias, symptoms indicative of hypotension or heart failure, hepatic and skin reactions.
- To consult their physician if they become pregnant while taking Matzim LA (diltiazem hydrochloride) extended-release tablets or plan to become pregnant.



